Talk Overview
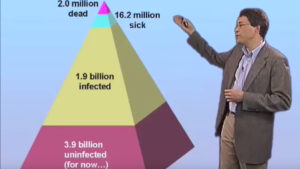
Human population growth and urbanization have accelerated dramatically in recent centuries, providing unprecedented opportunities for microbes that use our bodies as vehicles for their own propagation and transmission. These conditions have led to the emergence of virulent new pathogens and the increased prevalence of “classic” scourges, such as Mycobacterium tuberculosis. This tenacious microbe is transmitted via infectious aerosols produced by individuals with pulmonary tuberculosis. Infection is lifelong and symptomatic tuberculosis may develop following a period of clinical latency lasting for months, years, or decades. The first part of this lecture provides an overview of the natural history of TB infection and the global impact of TB on human health.
Tuberculosis remains one of the most important causes of human disease and death despite the introduction of vaccination in 1921 and chemotherapy in 1952. Although these interventions are inexpensive and widely available their impact is limited. The effectiveness of vaccination is unclear; in clinical trials, the protection conferred by vaccination has been variable and generally poor. Although chemotherapy can be highly effective, multiple drugs must be administered for 6-9 months to provide a reliable cure; the majority of tuberculosis patients are unable or unwilling to complete such a demanding regimen unless closely supervised. The second part of this lecture will discuss the challenges facing development of more effective vaccines and drugs for prevention and treatment of tuberculosis.
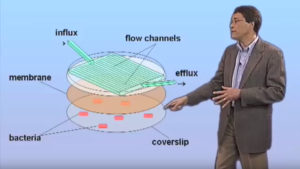
The principal obstacle to successful treatment of tuberculosis is the lengthy duration of current regimens, which require administration of multiple drugs for 6-9 months. The requirement for prolonged therapy is attributed to sub-populations of bacillary “persisters” that are refractory to antimicrobials. The persisters are not drug-resistant in the conventional (heritable) sense and it is a mystery why they are spared whilst their genetically identical siblings are killed. The third part of this lecture describes recent work in our laboratory using microfluidics and time-lapse microscopy to analyze the behavior of drug-stressed bacteria at single-cell resolution. These studies challenge conventional views of how antimicrobials kill (or fail to kill) bacteria.
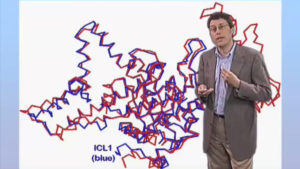
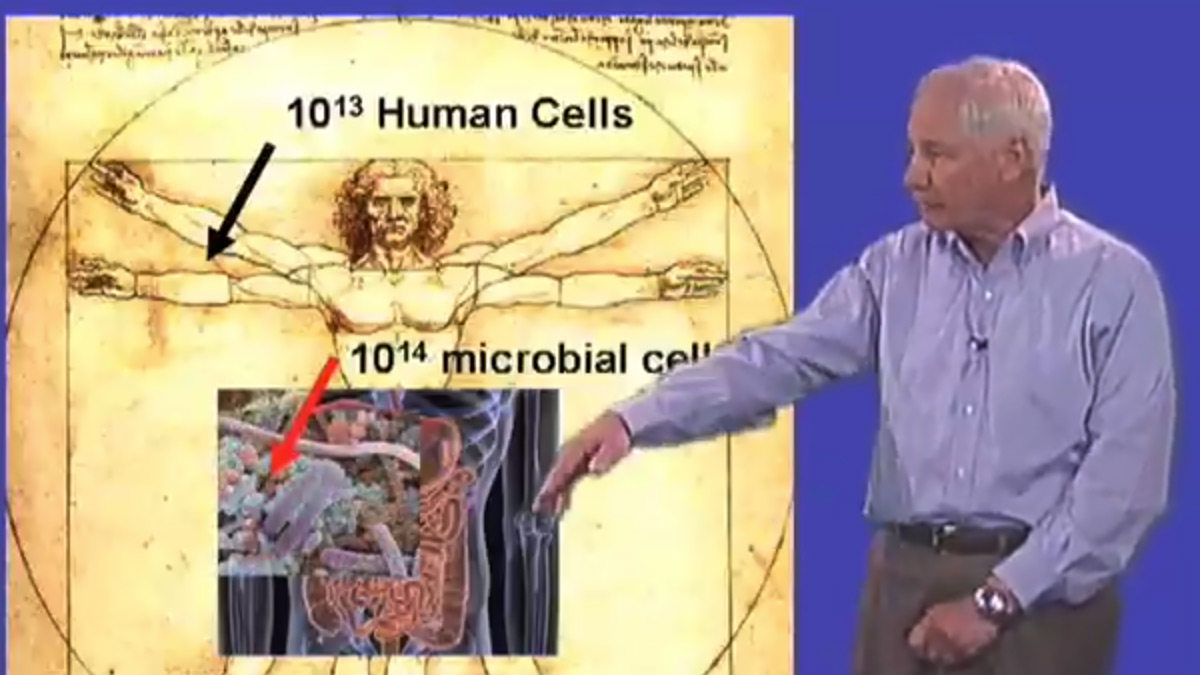
All pathogens must acquire and assimilate nutrients from their hosts in order to grow and multiply — our tissues are literally their food — yet surprisingly little is known about this fundamental aspect of the pathogenic lifestyle. Accumulating evidence suggests that M. tuberculosis might utilize fatty acids as its principal carbon and energy source during infection. The fourth part of this lecture describes work in our laboratory that is focused on identifying the metabolic pathways that are essential for growth and persistence of M. tuberculosis in vivo. Some of these pathways are potentially interesting targets for antimicrobial drug development, as they are not found in human cells.
Speaker Bio
John McKinney

John McKinney is Professor of Bacteriology at the École Polytechnique Fédérale de Lausanne (EPFL) in Switzerland. McKinney received B.A. (biology) and B.Sc. (genetics) degrees from The Evergreen State College (1987) and a Ph.D. from The Rockefeller University (1994). After completing his postdoctoral studies in the laboratory of William Jacobs at the Albert Einstein College of… Continue Reading








Leave a Reply